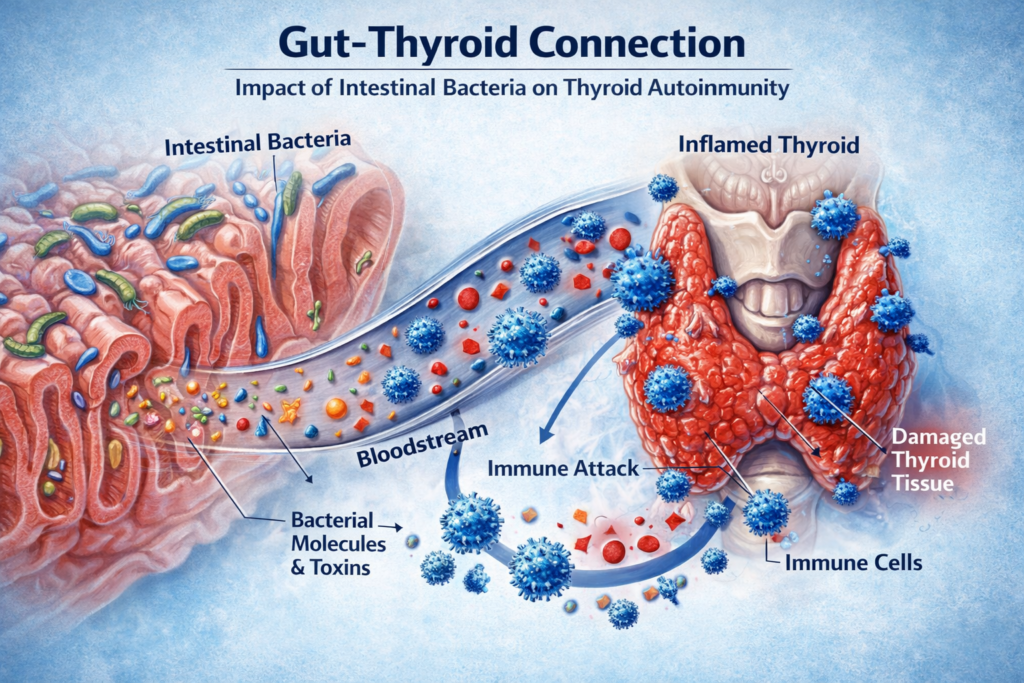
Scientists are increasingly discovering that the gut microbiome—the community of bacteria living in the digestive system—may play a significant role in autoimmune diseases, including Hashimoto’s thyroiditis.
A recent study investigated the presence of lipopolysaccharides (LPS) in the blood of patients newly diagnosed with Hashimoto’s thyroiditis. LPS are molecules produced by certain types of gut bacteria. When these molecules enter the bloodstream, they can trigger immune responses and inflammation throughout the body.
Researchers compared blood samples from people with Hashimoto’s thyroiditis to samples from healthy individuals. They found that patients with Hashimoto’s had significantly higher levels of circulating LPS, suggesting that bacterial toxins from the gut may be stimulating immune activity.
This finding supports the theory that a disrupted intestinal barrier—sometimes referred to as “leaky gut”—could allow bacterial components to escape from the digestive tract and activate immune cells.
When this happens, the immune system may become more likely to attack the body’s own tissues. In Hashimoto’s thyroiditis, the immune system targets thyroid cells, gradually damaging the gland and leading to hypothyroidism.
The researchers also examined dietary patterns and metabolic factors that might influence LPS levels and immune activation. Their results suggest that both gut health and diet could influence autoimmune activity in susceptible individuals.
Although the research does not prove that gut bacteria directly cause Hashimoto’s disease, it strengthens the growing scientific consensus that autoimmune disorders often involve complex interactions between genetics, immune function, and the microbiome.
Future treatments for autoimmune thyroid disease may therefore include strategies that address gut health—such as microbiome-targeted therapies, dietary interventions, or medications designed to reduce inflammation triggered by bacterial toxins.
For patients living with Hashimoto’s thyroiditis, these findings highlight why researchers are increasingly studying the gut-immune-thyroid connection.
Understanding how gut bacteria influence autoimmune responses could eventually lead to new treatment approaches that address the root causes of autoimmune thyroid disease rather than only replacing thyroid hormone.
Key Patient Takeaway:
New research suggests gut bacteria and bacterial toxins may influence autoimmune activity in Hashimoto’s thyroiditis, opening potential pathways for microbiome-based treatments.
Original Article: https://www.mdpi.com/2039-7283/16/2/26